Hip Bursitis
Description
A “bursa” is a small jelly-like sac usually containing a small amount of fluid. Bursae are located throughout the body. The most important bursae are located around the shoulder, elbow, hip, knee and heel. A bursa functions as a cushion between bones and the overlying soft tissues. It helps reduce friction between the gliding muscles and the bone.
The point of the hip is called the greater trochanter. It functions as an attachment point for several important muscles that move the hip joint. The trochanter has a fairly large bursa overlying it. The bursa measures about 3 inches long, 2 inches wide, and 1/4 inch thick. This bursa occasionally becomes irritated or inflamed. This is a common cause of hip pain. When this occurs, the condition is called “hip bursitis” or “trochanteric bursitis.” Another bursa located on the inside (groin side) of the hip is called the iliopsoas bursa. When it becomes inflamed, the condition is also sometimes referred to as hip bursitis, but the pain is located in the groin area. It is treated in a similar manner as trochanteric bursitis, but is less common.
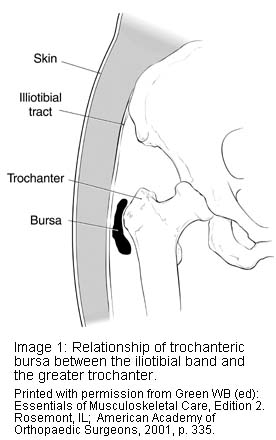
Diagnostic tests
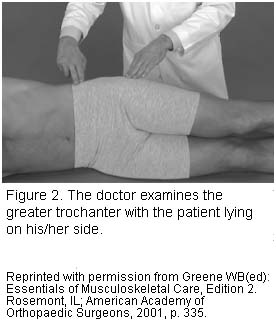
The primary diagnostic test is the doctor’s physical examination. The doctor will look for tenderness in the area of the point of the hip. He or she may request additional tests to rule out other possible injuries or conditions that could cause similar pain. These tests can include X-rays, bone scan and MRI (magnetic resonance imaging).
Risk Factors/Prevention
Trochanteric bursitis can affect anyone at any age. It is more common in women and in middle-aged or elderly people. It is less common in younger people and in men. The following circumstances have been associated with the development of hip bursitis:
Repetitive stress (overuse) injuries: These can include running, stair climbing, bicycling or standing for long stretches of time.
Injury to the point of the hip: This can include falling onto the hip, bumping your hip on the edge of a table, lying on one side of the body for an extended period, etc.
Spine disease: This can include scoliosis, arthritis of the lumbar (lower) spine and other spine problems.
Leg-length inequalities: When one leg is shorter than the other by more than an inch or so, this affects the way you walk and can irritate the bursa.
Rheumatoid arthritis: This makes the bursae more likely to become inflamed.
Previous surgery around the hip or prosthetic implants in the hip
Hip bone spurs or calcium deposits in the tendons which attach to the trochanter
Trochanteric bursitis can happen even when you don’t have any of these conditions.
Prevention is aimed at avoiding behaviors and activities that make the inflammation of the bursa worse. Some tips:
- Avoid repetitive activities that put stress on the hips.
- Lose weight if you need to.
- Get a properly fitting shoe insert for leg length differences.
- Maintain strength and flexibility of the hip muscles.
Symptoms
The main symptom is pain at the point of the hip. The pain usually extends to the outside of the thigh area and is usually described as sharp and intense in the early stages of the problem. After awhile, it may feel more “achy” and spread out. Typically, the pain is worse at night, when lying on the affected hip, and when getting up from a chair after being seated for a while. It also may get worse with prolonged walking, stair climbing or squatting.
Treatment Options
The initial treatment for hip bursitis does not involve surgery. Many cases of hip bursitis are treated effectively with simple lifestyle changes such as:
- Modifying activities (i.e., avoiding the activities that make it worse)
- Using non-steroidal anti-inflammatory medications (NSAIDs) to control inflammation and pain (i.e., ibuprofen, naproxen, piroxicam, celecoxib and others)
- Using a walking cane or crutches for a week or more when needed.
There is little evidence in clinical studies to support the use of physical therapy, but frequently patients will claim that it is helpful. The doctor may ask a physical therapist to teach you how to stretch the hip muscles and use “modalities” such as ice/heat, ultrasound or other treatments.
There are clinical studies that show an injection of corticosteroids along with a local anesthetic is helpful in relieving symptoms of hip bursitis. This is a simple and effective treatment that can be done in the doctor’s office. It involves a single injection into the bursa. The injection typically provides permanent relief, but on occasion the pain and inflammation may return and require another injection or two, given a few months apart. Often, the pain will be immediately relieved after the injection, and then return when the anesthetic wears off in several hours. The steroid takes a couple of days before it starts to work, so there may be a period of time where the pain seems to return and then again subside.
Use NSAIDs cautiously. Talk with your doctor about the NSAIDs you use. NSAIDs may have adverse side effects if you have certain medical conditions or take certain medications.
Treatment Options: Surgical
Surgery is very rarely needed for hip bursitis. In cases where the bursa remains inflamed and painful after non-surgical measures have been taken, and your doctor is certain that the diagnosis is correct, the bursa can be surgically removed. This involves giving you either general anesthesia (being put to sleep), or regional anesthesia (spinal anesthetic or nerve block with a sedative). A 3-inch to 4-inch incision is made over the bursa, and it is removed. Removal of the bursa does not hurt the hip and the hip can actually function normally without it.
A newer technique that is gaining popularity is removal (excision) of the bursa with arthroscopic surgery. This involves making two 1/4-inch incisions over the hip, and inserting a camera (arthroscope) in one incision, and a surgical instrument in the other to cut out the bursa. This surgery is much less invasive, and recovery is quicker and a little less painful. Both types of surgeries are done on an outpatient (day surgery) basis, so an overnight stay in the hospital is not usually necessary.
Following surgery, a short convalescence period can be expected. Most patients find that using a cane or crutches for a couple of days is helpful. It is reasonable to be up and walking around the evening after surgery. The soreness from surgery lasts for a variable amount of time, but usually resolves after a few days.
Research on the Horizon/What’s New?
More research needs to be done on the effectiveness of various non-surgical treatments for hip bursitis, such as NSAIDS, steroid injections, and physical therapy. There is currently research in progress in these areas. Early studies show arthroscopic excision of the bursa to be quite effective, but this is still currently being studied.
