Lumbar Spinal Stenosis
These articles are for general information only and are not medical advice. Full Disclaimer. All articles are compliments of the AAOS
Description
The lumbar spine (lower back) provides a foundation to carry the weight of the upper body. It also houses the nerves that control the lower body. With aging, the discs in the front of the spine become dehydrated. The joints in the back of the spine become overgrown due to arthritis. These degenerative changes are the result of the normal “wear-and-tear” associated with aging. Over time these changes can also lead to narrowing, or stenosis, of the spinal canal (see Figure 1).
Narrowing of the lumbar spinal canal pinches the nerves that control muscle power and sensation in the legs. Sometimes the pinched nerves become inflamed and cause pain in the buttocks and/or legs. These changes also can diminish the ability of the spine to carry the load of the upper body. They can lead to the forward slippage of one vertebra on another. This slippage, called “degenerative spondylolisthesis,” can cause both back and leg pain.

Your orthopedic surgeon can diagnose lumbar spinal stenosis using a combination of:
- Your symptoms
- Physical examination
- Plain X-rays
- Magnetic resonance imaging (MRI)
X-rays can show the presence of arthritis and slippage of the vertebrae. An MRI is used to determine whether nerves are being pinched. For people who cannot get an MRI (for example, people with pacemakers), a special test called a computed tomography (CT) myelogram may be necessary. This test requires the injection of a dye into the spine to make the nerves visible.
Risk Factors and Prevention
Lumbar spinal stenosis is usually caused by the wear-and-tear changes of aging. It usually affects middle-aged and older adults. People who are born with narrower spinal canals are more likely to develop this problem.
The best way to avoid the symptoms of lumbar spinal stenosis is to stay as physically fit as possible. Regular exercise can improve endurance and keep the muscles that support the spine strong. Avoiding weight gain can decrease the load that the lumbar spine has to carry. Patients should also avoid cigarette smoking. Both the smoke and the nicotine cause the spine to degenerate faster than normal.
Symptoms
Typically, patients with lumbar spinal stenosis have a long history of pain in the back, buttocks, or legs that gradually becomes worse. The symptoms are usually worsened by standing or walking upright. This results in achy pain, tightness, heaviness, and a sense of weakness in the buttocks and/or legs. These symptoms are generally relieved by sitting down or leaning forward. Although patients are unable to walk for very long, they may be able to ride an exercise bicycle for much longer. Some patients also find that it is easier to walk while leaning forward on a shopping cart. This position tends to create more space in the spinal canal. Leaning onto the handlebars of a bicycle creates the same effect. This relieves some of the pressure on the nerves.
Treatment Options
Non-surgical options to relieve the symptoms of lumbar spinal stenosis include:
A program of physical therapy with activity modifications. A program of gentle physical therapy may help. This program usually includes:
- Aerobic conditioning–the exercise bicycle is a good way for patients with lumbar spinal stenosis to workout without pain. Pool exercises can help people who cannot do aerobic exercises on land.
- Strengthening exercises
- Flexibility
- Other modalities
Anti-inflammatory medications–such as ibuprofen and naproxen–may be prescribed. These medications decrease pain and inflammation. Although they can be helpful, these medicines can have serious side effects. Prolonged use can lead to gastrointestinal ulcers, bleeding and kidney problems. Some of them may also increase the risk of heart attacks or strokes.
Epidural steroid injections. These injections deliver anti-inflammatory medication directly into the spinal canal and to the area of the inflammation. These injections are more effective than the medications taken by mouth. They may also have fewer side effects.
These injections deliver steroid medication straight to the nerve roots that are being pinched. Such steroid injections can give relief for weeks to months. They allow the patient to participate in more aggressive rehabilitation. In some cases, they may enable a patient to postpone or avoid surgical treatment altogether.
Bracing is generally not recommended for long-term use. If used for too long, bracing can lead to deconditioning of the muscles that support the back. Acupuncture or chiropractic manipulation can also be attempted.
All these nonsurgical treatments are aimed at decreasing inflammation. They also decrease the symptoms that patients experience. However, these treatments do not improve the narrowing of the spinal canal.
Treatment Options: Surgical
Most people with lumbar spinal stenosis do not require surgery. However, if patients are experiencing severe pain that limits their activities of daily living and their ability to have a good quality of life, surgery may be recommended. In general, surgery is only considered a last resort if all attempts at non-surgical therapies are unsuccessful and if the overall potential benefits of surgery are greater than the potential risks. Surgery may be recommended on an urgent basis if a patient has severe weakness or loss of bowel and bladder control.
The surgical procedure for lumbar spinal stenosis involves removing the bone and soft tissue that are pinching the nerves. This is called “decompression” or “laminectomy.” Some patients require only a decompression. However, patients with slippage of the spine or a curvature of the spine may require a stabilization procedure called fusion. In this procedure, two or more vertebrae are fused together using a bone graft harvested from the hip.
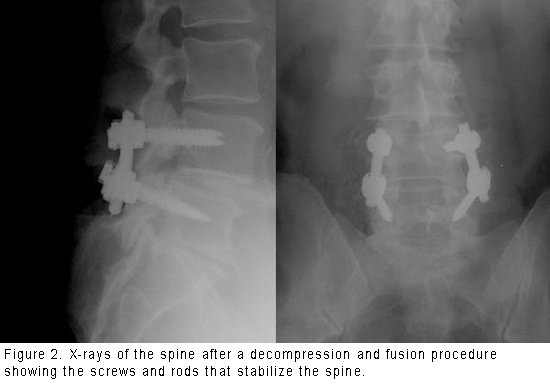
Fusion eliminates motion and prevents the slippage or curvature from worsening after surgery, which would cause more back and/or leg pain. Your surgeon may use screws and rods to hold the spine in place while the body heals the bone together (see Figure 2). Using screws and rods increases the rate of fusion and enables the patient to get out of the postoperative brace sooner. Overall the results of surgery are good to excellent in about 80 percent of patients. Patients tend to see better improvement of leg pain than back pain. Most patients are able to resume a normal lifestyle after a period of recovery from surgery.
There are some risks to surgery, including:
- Bleeding
- Infection
- Blood clots
- Reaction to anesthesia
- Tear of the sac covering the nerves (dural tear)
- Failure to relieve symptoms
- Return of symptoms after some time
- Failure of the bone fusion to heal
- Failure of screws or rods
- Need for further surgery
- Injury to the nerves
The risks of surgery depend on the patient and the exact procedure being performed. Elderly patients have higher rates of complications from surgery. So do overweight patients, diabetics, smokers, and patients with multiple medical problems.
After surgery, patients may be hospitalized for several days, depending on the patient and the procedure performed. Relatively healthy patients who only have a decompression procedure may be able to return home the same day. They usually return to normal activities after a few weeks.
Patients who have a fusion procedure are hospitalized for several days. They usually receive an outpatient physical therapy program. A lumbar corset or brace may also be prescribed after surgery. They return to normal activities after two to three months. Older patients who need more physical therapy may be transferred from the hospital to a rehabilitation facility.
Research on the Horizon and What’s New?
There are two areas of research that may change the way patients with spinal stenosis are treated. First, surgeons are developing ways to perform decompression procedures through smaller incisions. These techniques may cause less pain after the operation. They may allow quicker return to normal activities. Researchers are studying whether these new techniques are as effective and safe as traditional procedures.
Surgeons are also beginning to use manufactured bone-forming proteins to fuse the spine. These proteins replace harvesting bone from the patient’s hip. Harvesting a bone graft usually requires another skin incision. It can cause pain after the operation. However, the use of bone-forming proteins in the back of the spine for first-time surgeries is currently considered experimental. It is not approved by the U.S. Food and Drug Administration.
