Low Back Pain
These articles are for general information only and are not medical advice. Full Disclaimer. All articles are compliments of the AAOS
Description
Low back pain is one of the most common afflictions in our society. Almost every person will have at least one episode of low back pain at some time in his or her life. The pain can vary from severe and long-term to mild and short-lived. It will resolve within a few weeks for most people.
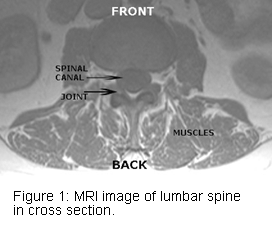
The low back (lumbar spine) is made up of five bones (vertebrae). The lumbar discs are between these bones in the front of the spine. They function as shock absorbers and allow for the motion of the lumbar spine. Behind the discs is the spinal canal (see Figures 1 and 2).
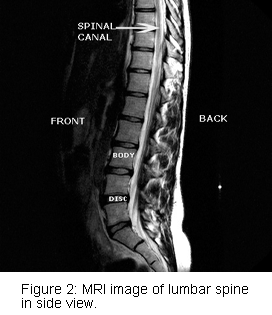
The spinal nerves run through this area and exit at each level of the spine. They are enclosed within the meninges, often referred to as the Dural sac. The Dural sac allows for the spinal nerves to travel through this area and stay within the spinal fluid. The lamina and the facet joints make up the back of the spinal canal. The lamina is a relatively flat area of bone that covers most of the back of the spinal canal. The facet (also called zygapophyseal or Z) joints are more to the side in the back and also allow for motion of the lumbar spine. They connect each vertebra to the one above and below it. Sticking backward from the lamina at each level of the spine is the spinous process. These are the bones that can be felt when you touch your back. The discs and nerves are too deep to be felt. The spinous processes function as an attachment point for a number of muscles. Many muscle groups surround the spine. They function to move and support the spine.
Cause
Doctors have many ideas about what causes low back pain, but no explanation applies to everyone. It may be related to damage to or aging of the disc, muscular problems, arthritis of the spine, problems with tendons or ligaments in and around the spine, or malpositioning of vertebrae. Low back pain is sometimes caused by:
- Excessive stress to the back, such as lifting something heavy.
- Minimal movement, such as bending or reaching for something.
Occasionally, it happens with no cause.
Diagnosis
See your doctor to diagnose low back pain. Tell him or her your complete medical history. The doctor will examine you physically. Often the physical exam is completely normal except for pain with motion. The doctor checks for:
- Evidence of nerve problems. The doctor evaluates strength, sensation, and reflexes. He or she may ask you to move your spine to see how limited the motion is.
- Another problem not related to the spine that could cause back pain, such as poor blood circulation. Tell the doctor what motions or positions hurt, and what helps relieve the pain.
If you have short-term (acute) back pain, the doctor may not order X-rays or other imaging studies; these are not likely to help in diagnosis or treatment. When X-rays are used, they are often normal or they show an abnormality that may or may not be related to the pain. (For instance, it is very common to see some disc degeneration in X-rays of people with back pain. But it is also very common to see it in people who do not have back pain. It is difficult to tell whether the degeneration is actually the cause of the pain.) The same is true for magnetic resonance imaging (MRI) and computed tomography (CT) scans.
X-rays and other studies are more likely to be helpful when low back pain does not get better on its own after a few weeks or a person has evidence of more severe problems. Tell the doctor if you have a history of a previous cancer, fevers, or chills that might be caused by an infection or a significant trauma like a fall or car accident that might have caused a fracture. Significant weakness on physical examination could also indicate problems. If a person is having trouble controlling their urine or bowels, the doctor will usually order X-rays and other studies more quickly.
The main purpose of X-rays is to look for an explanation for the pain. Many findings are considered to be nonspecific (they may or may not be related to the pain). Some of these non-specific findings are disc space narrowing, spurring, spina bifida oculta (incomplete formation of the lamina and spinous process), mild scoliosis, and a decrease in lumbar lordosis. Lumbar lordosis is the normal curvature of the spine when viewed from the side. When viewed from the front, the spine is normally straight. Discs are not visible on x-ray, only the disc spaces.
MRI (magnetic resonance imaging) is often the next imaging test ordered if the physician feels it is indicated. With MRI the doctor can see the discs and the nerves. He or she can see the level of degeneration of the discs and whether there is any material that has gone outside of the normal confines of the disc (herniation). MRI is also very good at showing infections, tumors, and fractures. Although an MRI can sometimes help the doctor determine the source of a back problem, it also often shows nonspecific findings.
The doctor may also order CT scans which are similar to three-dimensional X-rays, bone scans to look for areas of possible infection, tumor, or fracture, and tests to see how well nerves in the arms and legs conduct electrical signals (EMG/NCV tests). If osteoporosis is a concern, bone density studies may be ordered as well. Osteoporosis by itself should not cause back pain, but fractures due to osteoporosis can.
Risk Factors and Prevention
Low back pain can happen after an injury, especially if there is a fracture of the spine. Some other factors associated with low back pain are smoking and long-term exposure to vibration. Obesity may also be related. Factors such as posture, the type of work one does, diet, and the amount of exercise, are not closely related to low back pain.
Doctors do not know why some people with acute back pain go on to suffer from long-term (chronic) low back pain. They also don’t know why some people go on to feel quite well between episodes of severe pain.
Symptoms
The symptoms of low back pain vary in some ways and are similar in others. Most people find that reclining or lying down will improve their pain and after their initial severe episode, many will be able to rest at night without severe pain. Most people are worse when they bend over to pick something up. Some get relief from arching backward (extending the back). Leg pain also can be part of the problem. The pain is most common in the back or outer side of the thigh and can go all the way to the foot. Pain that goes to the foot is called sciatica because it is pain that follows the course of the sciatic nerve. Sciatica is often made worse by coughing or sneezing.
With an acute episode, back pain can be very severe for a few days or a week, and then will often improve. By 2-4 weeks, the majority of people are much better. Individuals vary greatly in the length of time between episodes, the length of each episode and intensity of each episode, and how they cope with the pain.
Treatment Options
Treatments for back pain are multiple and varied. At times counseling and education about the problem to ease a person’s anxiety are enough to make it tolerable until the episode resolves. A few days of rest can often calm the pain down as well. Prolonged bed rest (more than 2 days to 3 days) is no longer generally recommended. Medications such as non-steroidal anti-inflammatory drugs (NSAIDs) or acetaminophen (Tylenol) can be helpful. Occasionally stronger medications such as muscle relaxants and narcotics are used for a short period.
Although there is minimal scientific evidence of their effectiveness in treating low back pain, back braces are commonly used. The most common is a corset-type brace that can be wrapped around the back and abdomen. People who use them sometimes report feeling better supported and more comfortable. Although there is little definite proof that they help, there is also little risk to using them.
Several treatments, called passive modalities are also used frequently. These are treatments in which the patient isn’t required to actively do anything. Passive modalities include heat, cold, massage, ultrasound, electrical stimulation, traction, and acupuncture. All of these measures can help some people with back pain. How long the benefit will be or what the chances are of receiving benefit from any of these treatments isn’t completely known.
Another form of passive treatment is spinal manipulation. There are many different practitioners of spinal manipulation, each with their own style of manipulation. This has also at times improved symptoms of back pain.
Injections are sometimes used as well. The most commonly used medications are local anesthetics and/or steroids. They are usually given either in the area that is felt to possibly be the source of the pain, such as into a muscle or facet joint, or around the nerves of the spine (an epidural or nerve root injection). Injections are occasionally placed into the disc, but this is done far less frequently.
The next more invasive type of procedure that is done for low back pain is the procedure aimed at removing or destroying the area that is felt to be causing the pain. Some examples of this are intra-discal electrothermy (IDET) in which a coiled wire is placed into the disc and then heated, and radiofrequency ablation (RFA). These are more invasive and because they do damage tissue, have a higher risk and potential for longer-term side effects than the other treatments. If successful, they can help a person avoid a larger surgery, but there is still controversy over exactly when and to whom these procedures should be offered.
What is generally felt to be most appropriate and effective for most people with back pain is a good course of exercise and stretching. Restoring motion and strength to a painful lumbar spine can be very helpful in improving pain. Although there is controversy as to what are the best spine exercises, it is generally agreed that exercise should be both aerobic (aimed at improving heart and lung function) as well as specific to the spine. Aerobic exercises include walking, jogging, swimming, bicycling, etc.
Instruction in lifting techniques can be helpful as well. Improperly bending over to lift can cause a large increase in strain on the low back. Proper lifting keeps the back straight while you bend with the knees.
Treatment Options: Surgical
Indications for Surgery
Surgery for low back pain should only be performed when several conditions have been met. The first is that nonsurgical treatment options have been tried and have failed. Surgery should not be done if an exercise program is effective but the person does not want to do it. The second condition is that the surgeon feels there is enough possibility that the individual patient will have a good chance of having a successful result with surgery. An example of this would be a person with severe degeneration at one level of their spine and normal findings at the other levels. Another factor that goes along with this is that low back pain, like many other pain problems, can be worse during times of stress. It may not be a good idea to commit to an operation like this when other major stressful events are occurring in one’s life. Occasionally, the back problem can become more tolerable once the stress is reduced. The final factor is that the patient must decide if they are having enough of a problem to undergo an invasive procedure that is not guaranteed to work.
Surgical Options
Historically, the most commonly performed operation for back pain has been spinal fusion. There are a variety of ways this is done but the basic idea is to take the painful segment of the spine and get it to become a solid piece of bone. This will eliminate motion and, in theory at least, if it doesn’t move, it shouldn’t hurt. This can be done through the back (posterior) or through the front (anterior), or sometimes both ways. Spinal fixation of some sort is often combined with some form of bone graft or bone substitute. Bone graft can either be obtained from another part of the skeleton such as the pelvis (autograft) or be donated bone that is processed and used in a spine fusion (allograft). The results of spine fusion for low back pain vary. A good result is a decrease in pain. It is very rare for someone to be completely out of pain after a spine fusion. Full recovery can take more than a year.
A newer technique that has recently been introduced in the United States is disc replacement. The procedure involves removing the disc and replacing it with artificial components, similar to what is done in the hip or the knee. Doing this lets the segment of the spine keep some flexibility and hopefully maintain more normal motion. The recovery time may be shorter than with spine fusion because the bone does not have to solidify. Although it has been used in Europe for several years, it has only recently been used in the United States. Early results are promising.
Currently, disc replacements are done through an anterior approach and are primarily done on the lower two discs of the lumbar spine.
Research on the Horizon and What’s New?
A great deal of research is being performed to help doctors understand and treat low back pain. Some of the more exciting research includes new forms of disc replacement that someday may be injectable and research into gene therapy that may someday allow doctors to alter the aging process of the spine.
